|
The sensitivity and specificity of these tests were variable in approximately 60-90% and 90-100% of cases, respectively, depending on the method used. The presence of AQP4 antibodies has been verified by various methods, including visualization of AQP4-antibody immunoprecipitates by western blotting, fluorescence immunoprecipitation assay (FIPA), ELISA, and cell-based indirect immunofluorescence assay (CIIFA). 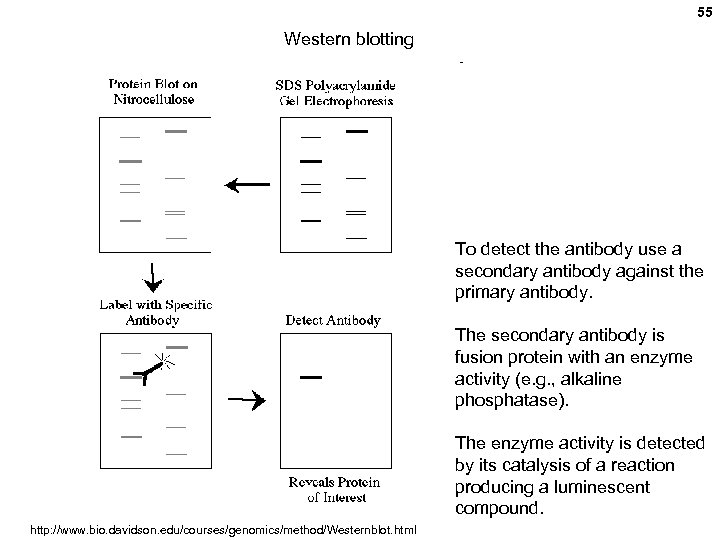
The target antigen of this autoantibody was quickly identified to be AQP4, the most abundant water channel in the CNS subsequently, the immunopathogenic role of AQP4 antibodies in NMO was reported. demonstrated that NMO-IgG was capable of specifically binding to CNS microvessels, pia mater, subpia mater, and Virchow-Robin spaces in rodent brain tissue by using an indirect immunofluorescence method. Treatments based on B cell- and antibody-depleting strategies such as rituximab administration and plasmapheresis have been effective in combination with conventional immunosuppressive treatment, in contrast to the inefficacy of these approaches for treating MS and other diseases associated with inflammatory lesions. 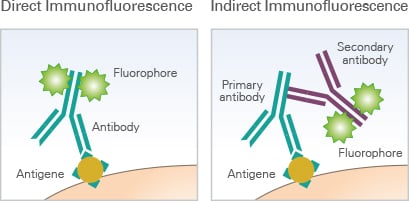
This evidence of autoantibody-mediated NMO pathogenesis enabled the development of therapeutic strategies targeted to the humoral arm of the immune system. An NMO-specific IgG, designated NMO-IgG, and antibodies to aquaporin-4 (AQP4) that serve as relevant antigens of NMO-IgG, are detectable in 60-90% of patients with NMO but are virtually absent in patients with MS and other inflammatory and non-inflammatory neurological diseases. However, recent reports suggest that NMO is a distinct disease entity with a fundamentally different pathogenic mechanism than that of MS or other demyelinating diseases. In particular, both NMO and multiple sclerosis (MS) have a relapsing-remitting course in the majority of cases, thus NMO has been typically considered to be a localized form of MS due to the lack of an NMO-specific laboratory test. These characteristics highlight the need to distinguish NMO from other demyelinating CNS conditions as early as possible however, it is often difficult to differentiate inflammatory demyelinating CNS disorders that have differing etiologies but similar clinical presentations and cerebrospinal fluid (CSF) and magnetic resonance imaging (MRI) findings. 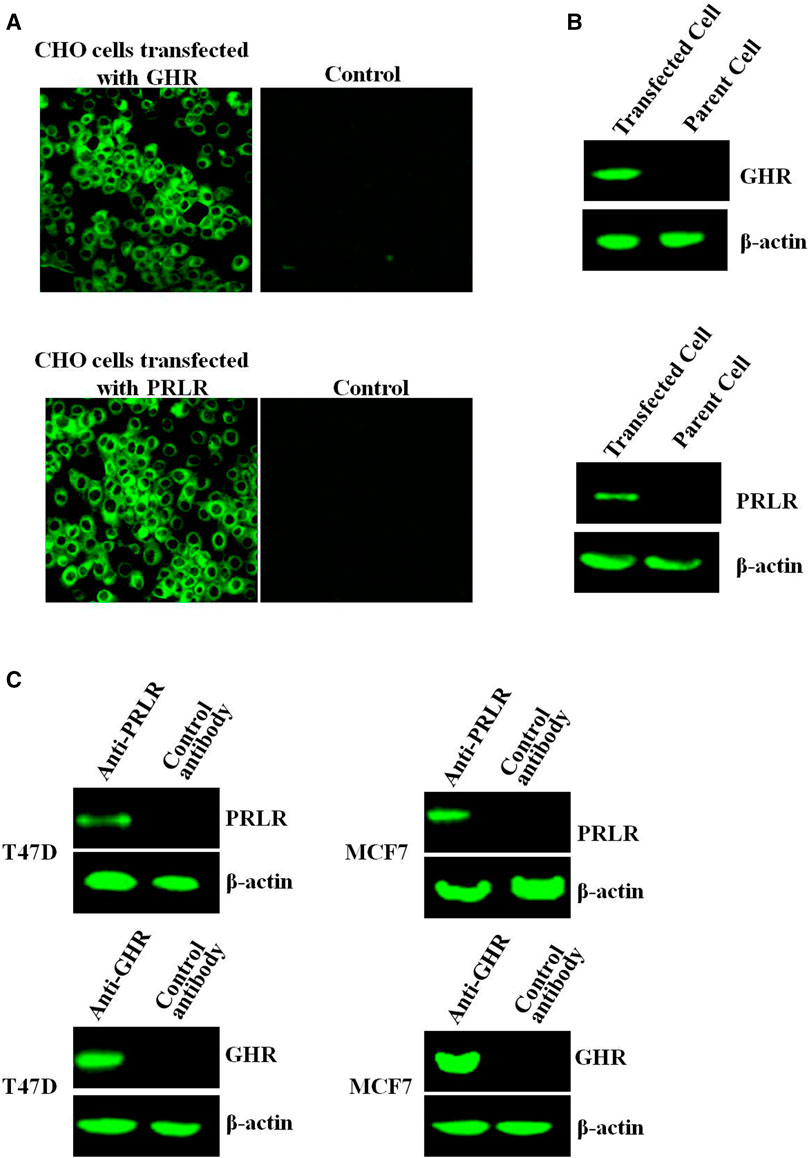
Due to its relapsing course with rare spontaneous remission, the accumulation of irreversible deficits and rapid progression of NMO often renders patients severely disabled. The condition which is considered to be a type of neuromyelitis optica spectrum disorder (NMOSD) includes NMO and an array of high-risk NMO disorders such as Asian optic-spinal multiple sclerosis (OSMS), recurrent myelitis associated with longitudinal extensive spinal cord lesions, recurrent isolated or simultaneous bilateral optic neuritis (RON/BON), and optic neuritis (ON) or myelitis/LETM in the context of certain organ-specific and non-organ-specific autoimmune diseases or with brain lesions typically observed in cases of NMO. It preferentially affects the optic nerves and the spinal cord, thus frequently manifests as recurrent optic neuritis (RON) and longitudinally extensive transverse myelitis (LETM). Neuromyelitis optica (NMO also known as Devic syndrome) is a chronic inflammatory demyelinating disorder of the central nervous system (CNS), which was first described in the late 19th century by E.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
